By now, most practitioners working with chronic illness, post-viral syndromes and Long Covid, or autoimmunity are familiar with Epstein–Barr virus, potentially even seeing it regularly in client histories or test results.
What I think is less clear is – what to do with it.
EBV generally doesn’t appear as a neat, isolated finding. Instead it emerges alongside fatigue that doesn’t resolve, relapsing symptoms under stress, immune dysregulation, or complex multi-system presentations.
Practitioners may recognise EBV as relevant — and still feel uncertain about how to ascertain its role – is it driving dysfunction? Or present because of immune dysfunction? Driver – or passenger?
EBV Reactivation is both a Symptom and a Teacher
Once infected, EBV is functionally part of the hosts immune system. They (the virus and the immune system) are no longer independent of each other.
EBV reactivation then, is a feature of the environment inside the body, it is shaped by immune capacity, physiological load, and environmental stressors.
The virus itself does not suddenly change behaviour without reason; rather, the immune system’s ability to maintain control shifts.
Think about it like a life-sentence prisoner. To be contained properly, there’s a lot of resources required: A prison building, electricity for the gates and cameras, food and clothing and resources for the prisoner, guards, and payment for the guards labour and more. It has to be accounted for in the budget for the county!
If there is an issue with resources – power outage, prison guards on strike due to not getting paid their wages, the walls aren’t maintained and crumble – the prisoner can escape and run riot.
This is why EBV frequently reappears during periods of:
- Chronic psychological or physiological stress
- Inflammatory or metabolic strain
- Hormonal transitions
- Immune exhaustion or repeated immune challenge
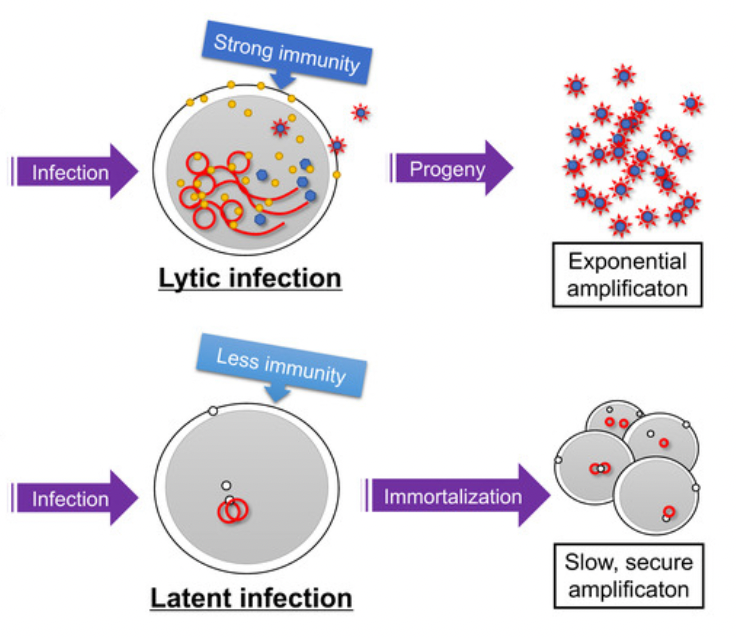
These all affect the ability of the immune system to keep EBV in tight latency. Sleeping peacefully and not causing havoc.
Instead, in these contexts, EBV may move into more active states — sometimes subtly, but sometimes symptomatically — without presenting as a classic acute infection.
EBV and Other Herpesviruses: A Shared Immune Burden
EBV belongs to the herpesvirus family, a family of 8 human viruses, and it’s pretty common to have more than one herpes virus on board.

These viruses share key characteristics:
- Lifelong latency
- Dependence on immune surveillance
- Sensitivity to immune exhaustion
When immune competence weakens, multiple latent viruses may become more active simultaneously, compounding immune load and symptom burden.
This is particularly relevant in clients with:
- Chronic fatigue syndromes
- Long COVID or post-viral illness
- Recurrent infections
- Autoimmune disease
In these cases, EBV is often part of a broader picture of impaired immune regulation, rather than a standalone driver.
EBV, Chronic Fatigue, and Post-Viral Illness
EBV is frequently implicated in chronic fatigue and post-viral presentations — not because it is always the original trigger, but because it can persist as an ongoing immune stressor.
Following an acute infection, some bodies fail to fully recalibrate immune function. Low-grade inflammation, altered cytokine signalling, and impaired cellular immunity can create conditions where EBV remains more active than expected.
Clinically, this may present as:
- Persistent fatigue disproportionate to exertion
- Post-exertional symptom flares
- Cognitive dysfunction or “brain fog”
- Poor stress tolerance
In these cases, addressing EBV in isolation rarely resolves symptoms. Instead, outcomes improve when we focus on restoring immune regulation, resilience, and recovery capacity.
Environmental and Physiological Stressors Matter
EBV reactivation is significantly influenced by both external and internal stressors that alter immune balance (both chronic and acute stress chemistry changes immune function considerably).
These may include:
- Psychological stress (EBV measures cortisol as a proxy marker for immune competence)
- Sleep disruption
- Hormonal shifts (puberty, postpartum, perimenopause)
- Metabolic instability
- Environmental exposures such as mould or toxins
- Acute infections (viral or bacterial)
These factors create an environment that is hospitable EBV reactivation, eroding immune resilience, making effective viral immune and cellular mechanisms more difficult to maintain.
This is why people can be stable for years before symptoms emerge — and why relapses often follow periods of cumulative stress or ‘being run down’.
Why EBV can feel so ‘un-straightforward’
Symptoms fluctuate.
Labs don’t always correlate neatly.
Interventions help some clients but not others.
The reason is not that EBV is unpredictable — it’s that immune systems are complex.
EBV acts within a dynamic system influenced by genetics, immune regulation, environmental load, and physiological capacity. Without accounting for these variables, EBV can appear confusing or contradictory.
This is also why protocol-based approaches often fall short. Without understanding why immune competence has weakened, interventions may provide temporary relief without long-term resolution.
A Shift in Clinical Perspective
Rather than asking, “How do I treat EBV?”, a more useful clinical question is:
“What is preventing this immune system from maintaining control?”
We are coming back to the Functional Medicine Framework that asks:
What is present in this body or this life that is getting in the way of healthy function?
AND
What is missing from this body or this life that is required for healthy immune function?
When EBV is viewed through this lens, it becomes less of a problem to eradicate and more of an important communication from the body.
It may point to:
- Immune depletion or exhaustion
- Loss of tolerance
- Cumulative physiological burden
- Systems operating at the edge of capacity
Understanding this allows us to intervene more strategically — supporting immune regulation, resilience, and recovery rather than chasing viral suppression alone.
Remember what I say all the time: We are not trying to OUTSMART the immune system – we need to understand what it is trying, but struggling, to achieve and then help it do that.
Where Deeper Understanding Is Needed
Recognising EBV patterns is an important first step.
This includes:
- Interpreting EBV markers in the context of the immune system
- Understanding co-factors and co-infections
- Recognising when EBV is likely driving symptoms — and when it is more of an opportunistic bystander
- Knowing when to intervene, when to stabilise, and when to step back
These nuances require a systems-based understanding of immune function over time.
Want to Go Deeper?
If EBV keeps appearing in your cases — particularly alongside chronic fatigue, post-viral illness, or complex immune presentations — learning to interpret context and co-factors is essential.Check out my free Functional Medicine Guide to Epstein-Barr Virus for Practitioners for more information on connecting the symptoms of EBV, testing, triggers, as well as how to manage constant reactivation.